Septoplasty
Septoplasty, the surgical treatment of a crooked or deviated nasal septum, is one of the cornerstones in improving functional breathing issues.
Where is the nasal septum?
The nasal septum is the dividing wall inside the nose that separates the nasal cavity into its two sides. The septum is made up of cartilage in the front of the nose and a thin sheet of bone toward the back of the nose. It is then covered by a skin lining layer on both sides. To get a better idea of what the septum is you can watch this video to see what the inside of the nose normally looks like, including a straight septum.
How a deviated septum develops
The septum can become deviated as a result of the normal nasal growth process or, more commonly, from nasal trauma. The patient below suffered several nasal fractures in the past which resulted in the deviation of her nose and septum, including her anterior septum. This caudal septal deviation is what causes the patient's asymmetric nostril size in this photo.
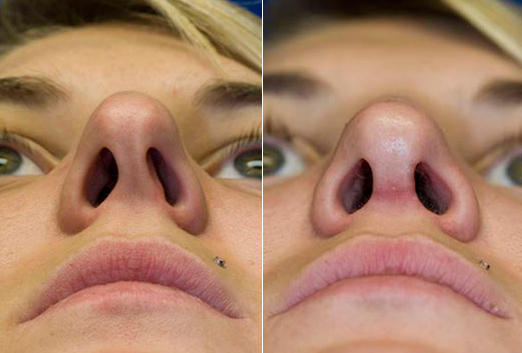
A deviated septum can be diagnosed by having a comprehensive nasal exam. Importantly, the more easily seen anterior septum may be straight, but the harder to examine posterior septum may be significantly deviated. This is one reason that Dr. Lamperti routinely assesses the entire nasal cavity using a small endoscope.
How can a deviated septum cause congestion?
Very few people have a perfectly straight septum, but more significant deviations of the septum can lead to a reduction in nasal airflow and the sensation of congestion. Even relatively small deviations of the septum from the midline can produce nasal blockage. This is especially the case where the septum meets the upper jaw by the floor of the nose since about 50% of nasal airflow occurs along the floor of the nose.
What does septoplasty surgery involve?
Septoplasty typically involves making a small incision hidden on the inside of the nose on one side. The photo below shows an intra-operative view of a patient's left nostril where the planned septoplasty incision line has been marked.
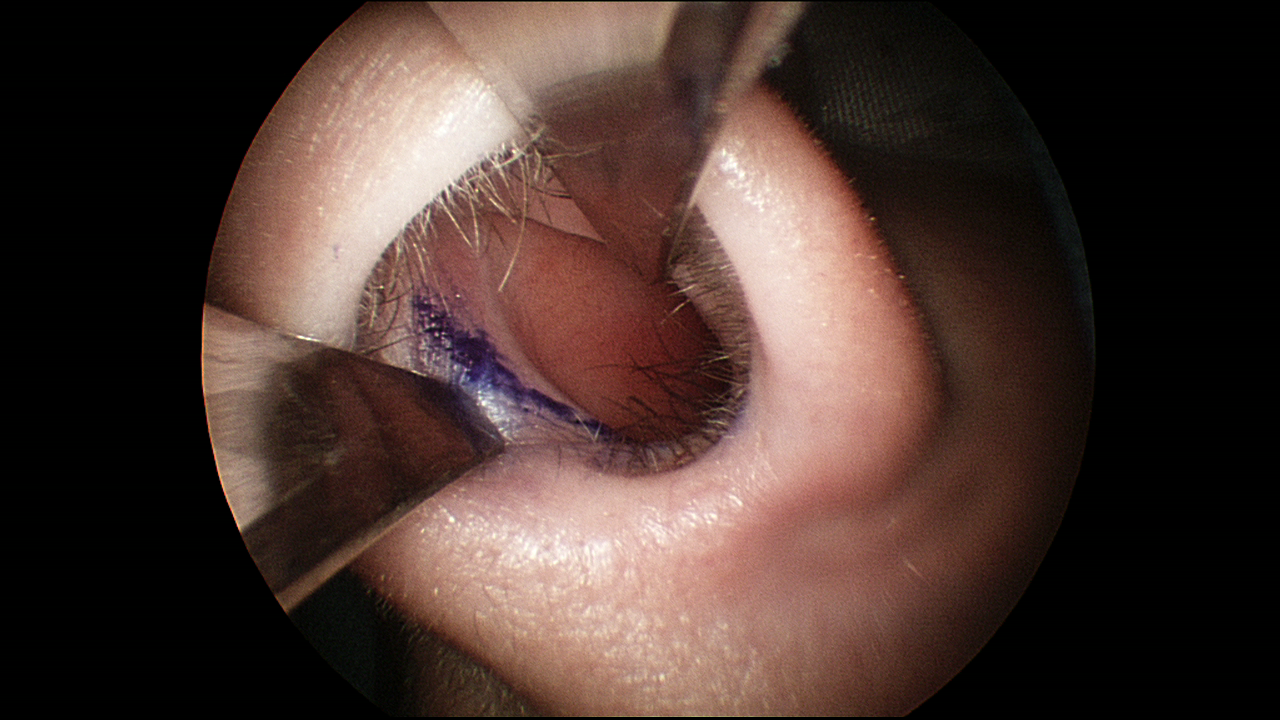
This allows Dr. Lamperti to gently elevate the skin lining off of the deviated cartilage and bone of the septum. The misaligned cartilage and bone is then removed which allows Dr. Lamperti to sew the skin lining back to itself using a quilting type suture. An L-shaped strut of cartilage is left in place to maintain normal nasal and tip support.
All the septoplasty sutures used are dissolvable and come out on their own. With the deviated cartilage and bone removed the skin lining is able to lay much straighter which then allows for smoother airflow when breathing. You can see a video of a septum before and right after septoplasty below:
Occasionally, in more complicated deviations, a small external incision is also used to allow for complete reconstruction of the septum. This is often the case if a portion of the L-strut is deviated. This was the approach used in the patient shown above who had a caudal septal deviation.
You can see how a septoplasty is performed from the surgeon's perspective here.
Septoplasty Frequently Asked Questions
How long does septoplasty surgery take?
Septoplasty surgery typically takes about 15 to 30 minutes. Of course, more complicated cases can take longer.
What kind of anesthesia is used for septoplasty?
Septoplasty surgery is done in the operating room. Either IV sedation or general anesthesia can be used. Once this anesthesia has been administered, Dr. Lamperti injects local numbing medicine that will last a couple hours. Surgery is done as a same-day outpatient procedure; you are able to go home once you have recovered from anesthesia.
Is nasal packing used during septoplasty?
Dr. Lamperti does not typically use packing after septoplasty surgery. Instead he uses dissolvable sutures to ensure that the septum heals correctly. Occasionally, Dr. Lamperti will use a thin plastic splint inside the nose to prevent scar band formation. This splint is removed one week after surgery.
Is septoplasty covered by insurance?
Septoplasty is medically covered surgery and is typically covered by insurance. If you like, Dr. Lamperti's office can find out if septoplasty is covered under your insurance plan.
How long is septoplasty recovery?
Septoplasty recovery is usually about 3 to 4 days and can often occur over a long weekend. The recovery for a more extensive septoplasty or septoplasty done in conjunction with rhinoplasty usually takes about 7 days.
What are the risks of septoplasty?
The risks of septoplasty include the risks of any surgery such as bleeding, infection, reaction to the anesthesia, and injury to surrounding structures. Risks specific to septoplasty include persistent congestion or asymmetric breathing. There is also a rare chance of a hole developing in the septum (septal perforation) during the healing process. Even more rare risks are that of injury to the smell organ or spinal fluid leak. Dr. Lamperti limits his manipulation of the upper boney portion of septum to avoid injury to the smell organ or bone of the skull base and has never had this complication occur in his practice.
Can I have a nose job during my septoplasty?
The time of your septoplasty is an ideal point to have a rhinoplasty to reshape your nose. Dr. Lamperti often uses portions of septal cartilage during rhinoplasty surgery to create the planned changes in the nose's appearance. The cartilage removed during an isolated septoplasty is otherwise left out of the nose, making it more difficult (though not impossible) to perform rhinoplasty in the future.
What about having sinus surgery along with a septoplasty?
Sinus surgery can be done at the same time as septoplasty. The decision to perform sinus surgery is based on a patient's symptoms and findings on sinus CT scan. It is important to understand that sinus surgery itself will not affect nasal airflow.
Can septoplasty help with my snoring or sleep apnea?
Improving nasal breathing can, in certain situations, help with symptoms of snoring or sleep apnea. This occurs as you are able to do less mouth breathing while sleeping. Septoplasty is not a cure-all, however, and may not affect your sleep symptoms at all. Dr. Lamperti can assess your situation during your consultation to let you know whether nasal surgery has a chance of improving your sleeping issues.

Meet Plastic Surgeon, Dr. Lamperti
Dr. Lamperti, a Seattle rhinoplasty super-specialist, has devoted his career to treatments of the head, face and neck. He feels that by focusing his plastic surgery endeavors solely to the face he is best able to provide the excellent results his patients desire.
Interested in learning more about having a Rhinoplasty Treatment in Seattle with Dr. Lamperti?
Contact us to have a private consultation or view Before & After photos here.